Chloramphenicol: what it is and when it's used
Chloramphenicol is a broad-spectrum antibiotic used for serious infections when safer drugs fail. It works by blocking bacterial protein production, so germs stop reproducing. You’ll see it most often as eye drops or ointment for bacterial conjunctivitis, but doctors sometimes give it by mouth or IV for severe infections like meningitis, rickettsial diseases, or life‑threatening anaerobic infections.
Why is it not used more often? Because it can cause serious blood problems. Two different bone marrow effects matter: a reversible marrow suppression that usually clears after stopping the drug, and a rare, unpredictable aplastic anemia that can be permanent and fatal. That’s why systemic chloramphenicol is reserved for cases where alternatives aren’t suitable.
Safety basics and warnings
If your doctor prescribes systemic chloramphenicol, expect blood tests before and during treatment. A baseline complete blood count (CBC) and periodic monitoring help catch marrow suppression early. Watch for signs like unusual bruising, bleeding, persistent sore throat, or extreme tiredness, and report them right away. Never give chloramphenicol to newborns unless a specialist recommends it — infants can develop “gray baby” syndrome, a serious condition from poor drug clearance that can cause low blood pressure and breathing problems.
Chloramphenicol can also interact with other medicines. It may increase levels of drugs cleared by the liver, such as warfarin or phenytoin, so doctors check for interactions and adjust doses as needed. Side effects beyond blood issues include nausea, diarrhea, and rare nervous system effects like optic neuritis. Topical eye use carries a lower risk but still needs proper diagnosis and the right product.
Practical tips if you need it
Ask why your prescriber chose chloramphenicol and how long treatment will last. For topical eye drops, follow the exact dosing and avoid sharing bottles. For oral or IV therapy, stick to the schedule and don’t stop early without talking to your clinician — stopping too soon can let the infection come back. If you have a history of blood disorders, liver problems, or are pregnant, bring that up before starting the drug.
Resistance is a thing here too. Some bacteria make an enzyme that inactivates chloramphenicol, so cultures and sensitivity tests guide use in hospital settings. That’s another reason why doctors prefer targeted therapy over broad use.
Forms include topical drops, oral tablets, and IV solutions. Topical eye products are common and usually safe for short courses. Systemic use is strictly controlled: hospitals prescribe it for confirmed resistant infections or when the bug is known to respond. Treatment length depends on the infection — days for minor infections, weeks for severe ones — and doctors balance benefit versus bone marrow risk. Always tell your clinician about current medicines and allergies. If blood work shows falling counts, they switch therapy fast to prevent complications.
Ask your provider questions.
Bottom line: chloramphenicol is effective and sometimes life‑saving, but it carries risks that need careful monitoring. Use it when necessary, under close medical supervision, and report any worrying symptoms without delay.
In one of my recent research findings, I discovered that Chloramphenicol has shown promising results in the treatment of Whipple's Disease. This rare bacterial infection affects the digestive system and can cause various complications if not treated effectively. The use of Chloramphenicol has proven to be a reliable choice due to its excellent penetration into affected tissues and its ability to target the causative bacteria, Tropheryma whipplei. However, it's essential to note that the treatment duration can be long, requiring up to a year or more of therapy. With that being said, it's crucial to consult with a medical professional before considering Chloramphenicol as a treatment option for Whipple's Disease.
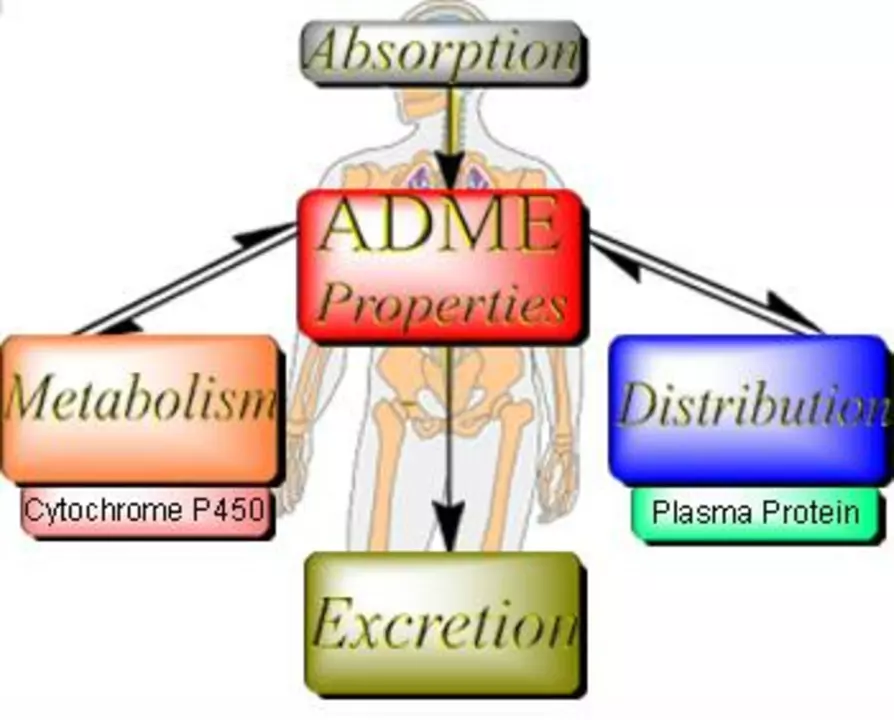
I recently delved into the fascinating topic of the pharmacokinetics of Chloramphenicol, specifically how it's metabolized and excreted in our body. Chloramphenicol, an antibiotic, is absorbed and distributed throughout our body, mainly binding to plasma proteins. It's primarily metabolized in the liver, where it undergoes glucuronidation, converting it into inactive metabolites. These metabolites are then excreted through the kidneys via urine. It's truly amazing to learn about how our body processes this powerful antibiotic and safely eliminates it from our system.