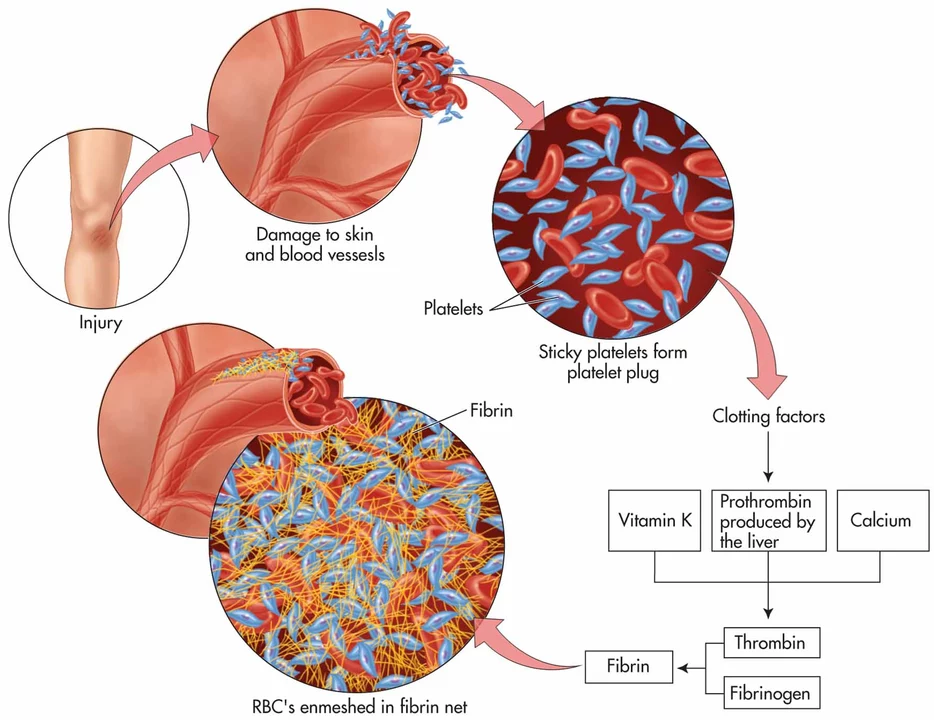
Blood clotting tests: what you need to know
Blood clotting tests check how fast your blood forms clots and how well the system that stops bleeding works. Doctors order them when someone has unusual bleeding, easy bruising, a clot like DVT or PE, before surgery, or when taking blood thinners.
Common tests and what they mean
PT (prothrombin time) measures the clotting pathway linked to factors made by the liver and affected by warfarin. Results often come as INR (international normalized ratio). A normal INR is about 0.9-1.2 for people not on warfarin. People on warfarin usually target 2.0-3.0 for many conditions; some need higher targets.
aPTT (activated partial thromboplastin time) checks another clotting pathway. It's used to monitor heparin therapy and to screen for inherited clotting problems. A long aPTT can mean factor deficiencies, inhibitors, or anticoagulant effects.
Platelet count tells how many platelets you have. Low platelets raise bleeding risk. Very high platelets can raise clot risk. Normal range is roughly 150,000-450,000 per microliter.
D-dimer is a fragment released when a clot breaks down. A normal D-dimer makes large clots unlikely. An elevated D-dimer can mean recent clotting, inflammation, infection, or recent surgery. It's useful in emergency settings to rule out deep vein thrombosis or pulmonary embolism when combined with clinical assessment.
Fibrinogen measures a key protein for clot formation. Low fibrinogen may cause bleeding; high fibrinogen can be a marker of inflammation or clotting risk.
Preparing for tests and things that affect results
No general fasting is required for these tests. Bring a list of all medicines and supplements. Blood thinners like warfarin, heparin, apixaban, rivaroxaban, dabigatran, and aspirin affect results and must be reported. Certain antibiotics, herbal products, and liver disease also change values.
If you take warfarin, your clinic may ask about diet changes and follow INR more often after starting or stopping other meds. For heparin, aPTT is the monitoring test. Point-of-care INR devices exist and are handy for people who self-monitor.
Results need context. One abnormal value often leads to repeat testing or additional tests like factor assays, mixing studies, or imaging for suspected clots. If D-dimer is high and symptoms suggest a clot, your doctor will likely order an ultrasound or CT scan.
Seek immediate care for heavy bleeding, sudden severe headache, new weakness, trouble speaking, or breathing problems. For high INR with bleeding, emergency reversal may be needed.
Simple steps help keep testing accurate: avoid alcohol right before a test, tell the lab about recent blood transfusions, and follow your provider's instructions about stopping or continuing medicines before testing. Keep copies of your key results—knowing your baseline helps future care.
If you are pregnant or planning pregnancy, tell your provider. Pregnancy changes clotting tests; conditions like preeclampsia and HELLP affect results. Children have different normal ranges, so labs compare to age-specific values. If you travel on blood thinners, carry a card listing your medication and INR. Communicate with the lab about urgent testing and same-day results if you have active symptoms today.
As a blogger, I recently researched blood clotting tests and wanted to share some key takeaways with you. These tests are crucial in diagnosing clotting disorders and monitoring treatment effectiveness. When preparing for the test, you should inform your doctor about any medications you're taking, as some can influence the results. It's also important to follow any specific instructions given by your healthcare provider. Overall, the process is relatively simple, typically involving a blood sample drawn from a vein in your arm, and results are usually available within a few days.