The 80-125% Rule: Understanding Bioequivalence Confidence Intervals
The 80-125% rule determines bioequivalence between generic and brand-name drugs. Learn what this range really means for patient safety and why confidence intervals matter.
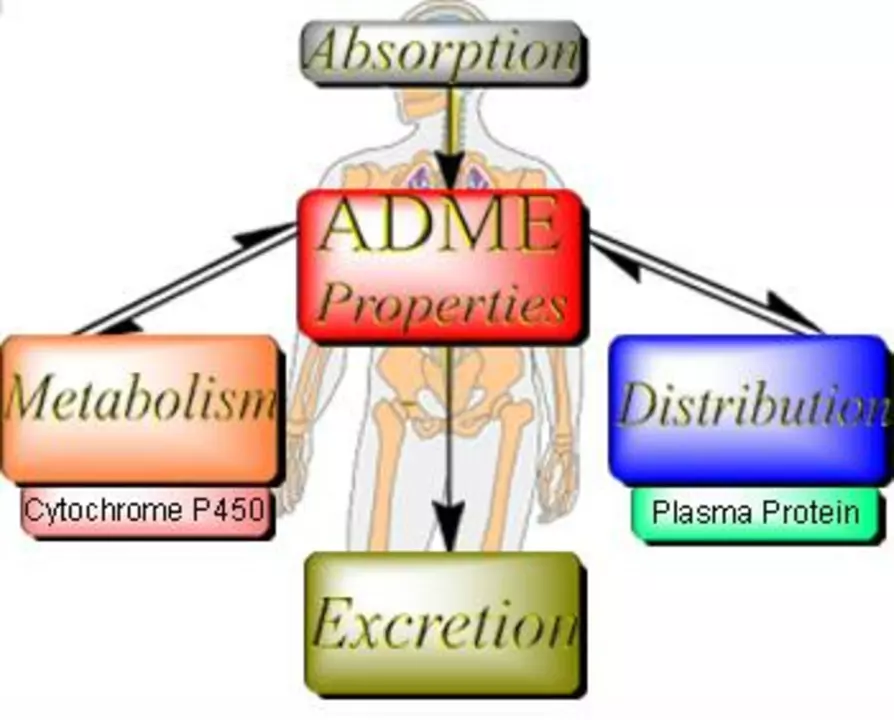
Pharmacokinetics explains what happens to a drug from the moment you take it until it's out of your system. Understanding absorption, distribution, metabolism, and excretion (ADME) helps you pick the right dose, time medicines correctly, and avoid nasty interactions. This is useful whether you're reading about metformin alternatives, buying antibiotics like moxifloxacin, or comparing blood pressure drugs such as enalapril.
Absorption decides how much of the drug reaches your bloodstream. Pills, creams, injections and patches are absorbed differently. For example, topical minoxidil acts locally on the scalp while oral simvastatin (Zocor) needs to pass through the gut and liver first. Food, stomach pH, and other meds change absorption — taking certain antacids or fiber with a pill can cut how much gets absorbed.
Distribution is where the drug travels. Blood flow, body fat, and protein binding matter. Some drugs stick to proteins in the blood and act slowly; others move freely into tissues. That explains why a dose that works for one person may feel weak or strong for another. Older adults and people with low albumin can see different drug levels than younger, healthy adults.
The liver changes many drugs into forms your body can use or remove. Enzymes like CYP3A4 and CYP2D6 do most of the work. If you take a drug that blocks these enzymes, levels of other drugs can rise and cause side effects. For instance, combining some cholesterol meds with strong enzyme blockers raises risk of muscle problems. Genetics also affect metabolism — some people process drugs fast, others slow — which is why doctors adjust doses.
Excretion removes drugs through urine, bile, or feces. Kidney function controls how long many drugs stay in your body. If kidneys are weak, drugs like certain blood pressure medicines or antibiotics can build up unless doses are reduced. That’s why doctors check kidney tests and why seniors often need lower doses. Time between doses depends on a drug’s half-life — drugs with long half-lives need fewer daily doses.
Why should you care? A basic grasp of pharmacokinetics helps you avoid mistakes when ordering meds online, like mixing drugs that interact or choosing the wrong form of a medicine. Articles on our site about checking pharmacy credentials, safe steroid purchases, and drug alternatives all link back to pharmacokinetics. Knowing the core ideas helps you read those pieces and make smarter choices.
Practical tips: always tell your pharmacist about all medicines and supplements you use, follow fasting or food instructions on labels, and ask if kidney or liver issues affect dosing. If you switch brands or buy from a different online pharmacy, check if the formulation or strength is the same — small changes can matter.
Pharmacokinetics isn’t a mystery. Learn these basics and you’ll understand why doctors change doses, why some drugs need timing, and why interactions happen. That knowledge makes reading drug guides and shopping for meds on InternationalDrugMart.com far safer and more useful. Ask questions if something feels unclear.

The 80-125% rule determines bioequivalence between generic and brand-name drugs. Learn what this range really means for patient safety and why confidence intervals matter.
I recently delved into the fascinating topic of the pharmacokinetics of Chloramphenicol, specifically how it's metabolized and excreted in our body. Chloramphenicol, an antibiotic, is absorbed and distributed throughout our body, mainly binding to plasma proteins. It's primarily metabolized in the liver, where it undergoes glucuronidation, converting it into inactive metabolites. These metabolites are then excreted through the kidneys via urine. It's truly amazing to learn about how our body processes this powerful antibiotic and safely eliminates it from our system.